Medical Tests for CI users
Broken bones, ruptured tendons, artery calcification or a suspected tumors – there are many reasons why medical professionals want to get the inner pictures of their patients’ organs. The users of MED-EL hearing implants are well prepared for this.
Unlike normal light, X-rays penetrate human tissue, casting shadows on dense tissue types. Captured on a film strip, this shows a shadow image of the bone structure. This method is generally not suitable for imaging soft tissue.
The classic tomograhy and CT
In X-ray examinations, if the radiation source and filming surface are moved closer to each other during the exposure, only a thin area in focus remains sharp. Higher and deeper levels are blurred into a gray veil, and instead of a shadow image, a kind of stamp impression of the examined level is produced. This is referred to as a tomographic image. The relatively long recording time in the classical method caused high radiation exposure.
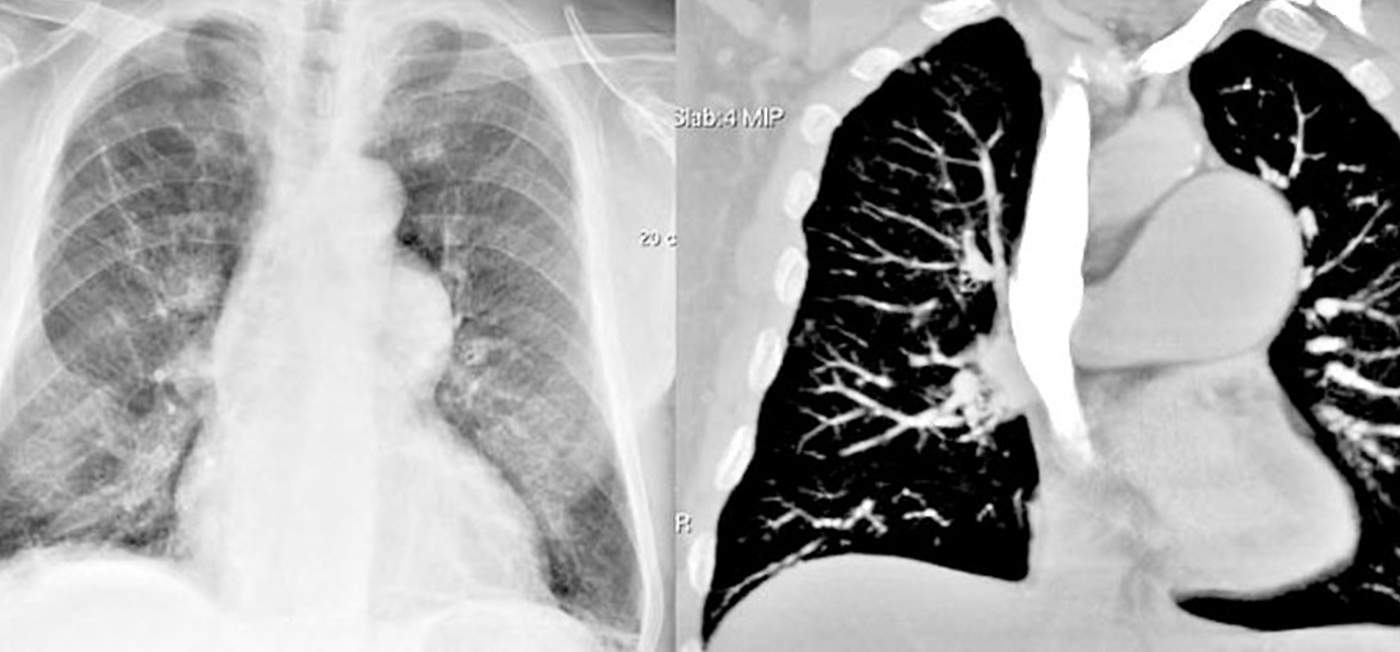
Today, images of several layers can be created during a single exposure controlled by a computer. The thickness of each slice can be limited to tenths of a millimeter and overall radiation exposure can be kept low. Computed tomography CT has completely replaced classical tomography.
The alternatives for organ imaging
In scintigraphy, radioactive substances are briefly introduced into the organ under examination. X-ray or CT images can then be used to examine the function of this organ. Emission computed tomography (ECT) and positron emission tomography (PET) are special forms of scintigraphy.
Sonography uses ultrasound, high-frequency sound waves of 1 to 40MHz. It can be used to examine organs containing fluids. The comfortable and safe procedure can be used without hesitation even during pregnancy. The images are less accurate than with CT or MR. Gases, e.g. in lungs or intestines, interfere with ultrasound images, as well as bones – an effect that is sometimes deliberately used for imaging.
Imaging techniques using infrared radiation or measurement of electrical impedances are only rarely used. More common procedures are those in which a tiny camera is inserted into body orifices to obtain an image of the inside of the body – as in gastroscopy of the stomach.
Implants and magnetic resonance imaging
The high magnetic forces in MR impose limitations on implant users. The Austrian manufacturer MED-EL is a pioneer in producing MR-capable hearing implants.
For some implants, special safety precautions must be observed during MR examinations. Implants from some manufacturers require surgical intervention before and after the examination. Despite compliance with all regulations, complication rates of over 50 percent have been reported with some systems – sometimes even leading to explantation of the CI.
Users of MED-EL hearing implants are on the safe side! With the exception of the VORP 502 middle ear implant used in the past, all MED-EL hearing implants are MR-safe up to 1.5 Tesla, and the SYNCHRONY implants are even MR-safe up to 3.0 Tesla – the unique magnet design in the SYNCHRONY makes this possible.
Users of MED-EL implants have only rarely reported an unpleasant feeling in the MR and have not experienced any serious complications from an MR.
In case of a possible MR examination, the examining staff should be informed about the implant when making the appointment. This way there is enough time until the appointment for possible questions to the manufacturer of the implant.
Implants and diagnostic imaging
Ultrasound treatments in the cranial region, such as ultrasonic tooth cleaning, are not recommended for hearing implant users. Ultrasound scans of the trunk and extremities are safe.
CTs make almost half of all imaging examinations in Germany and this proportion is probably similar in Austria. Luckily, CTs can be performed on implants without hesitation, just as the other X-ray examinations. In many implantation clinics, the position of the implant is even routinely checked by X-ray.
The number of MR examinations is rising internationally, and devices with stronger magnets are being used increasinly. Therefore, clinicians now recommend hearing implants that allow risk-free 3T MR examinations.






