Modern medicine can preserve future opportunities!
Promising developments in gene therapy for hearing loss are giving hope. But what does this mean specifically for those affected today?

About half of all congenital hearing disorders are genetic, the most common being Connex-26 deafness. More than 200 different genetic causes of congenital hearing disorders have been identified so far. Otoferlin deafness, which is comparatively rare, affects only 2 to 8% of all congenital hearing impairments caused genetically. However, for this relatively small group with a mutation in the OTOF gene, promising gene therapy is currently being tested.
The first encouraging results are giving hope to hearing-impaired people in general and to their families. However, this therapy can only help a small number of children with hearing loss, and it is currently only available as part of a scientific study at the few participating clinics worldwide. As promising as therapy may be, people with hearing impairment today – especially children – need rapid intervention. They cannot wait for future developments! But with the latest technology, you can keep your future possibilities open.
Deaf and hard of hearing people can’t wait!
Numerous studies show that the earlier children born deaf are implanted with cochlea, the better the hearing outcomes with the implant![1]

Photo: Adobe Stock
The developmental window during which children can acquire spoken language lasts roughly until they reach school age. After that, they can still expand their vocabulary, learn grammar structures or foreign languages. However, if a child has not been exposed to the basic concept of spoken language by that age, acquiring spoken language later becomes much more difficult and only partially possible. The development of other auditory abilities – such as sound localization or picking out a single sound source from a complex environment — also depend on time‑limited developmental windows.[2]
However, even with the adults who later become deaf, prompt intervention leads to much better hearing outcomes. This is due to cognitive changes that begin to occur with the onset of deafness[3].
For people who are deaf or hard of hearing today, every single day makes difference! Therefore, they benefit best from rapid interventions using the currently available options: In the case of profound hearing loss or deafness, these are usually cochlear implants.
The Current State of Gene Therapy for Hearing
Children with otoferlin deafness have normally formed inner ears with normally developed hair cells. However, because these hair cells lack the protein otoferlin, they cannot release the neurotransmitter needed for hearing. With the new gene therapy, a surgeon injects a carrier virus into the inner ear. This virus delivers the missing genetic information into the hair cells.
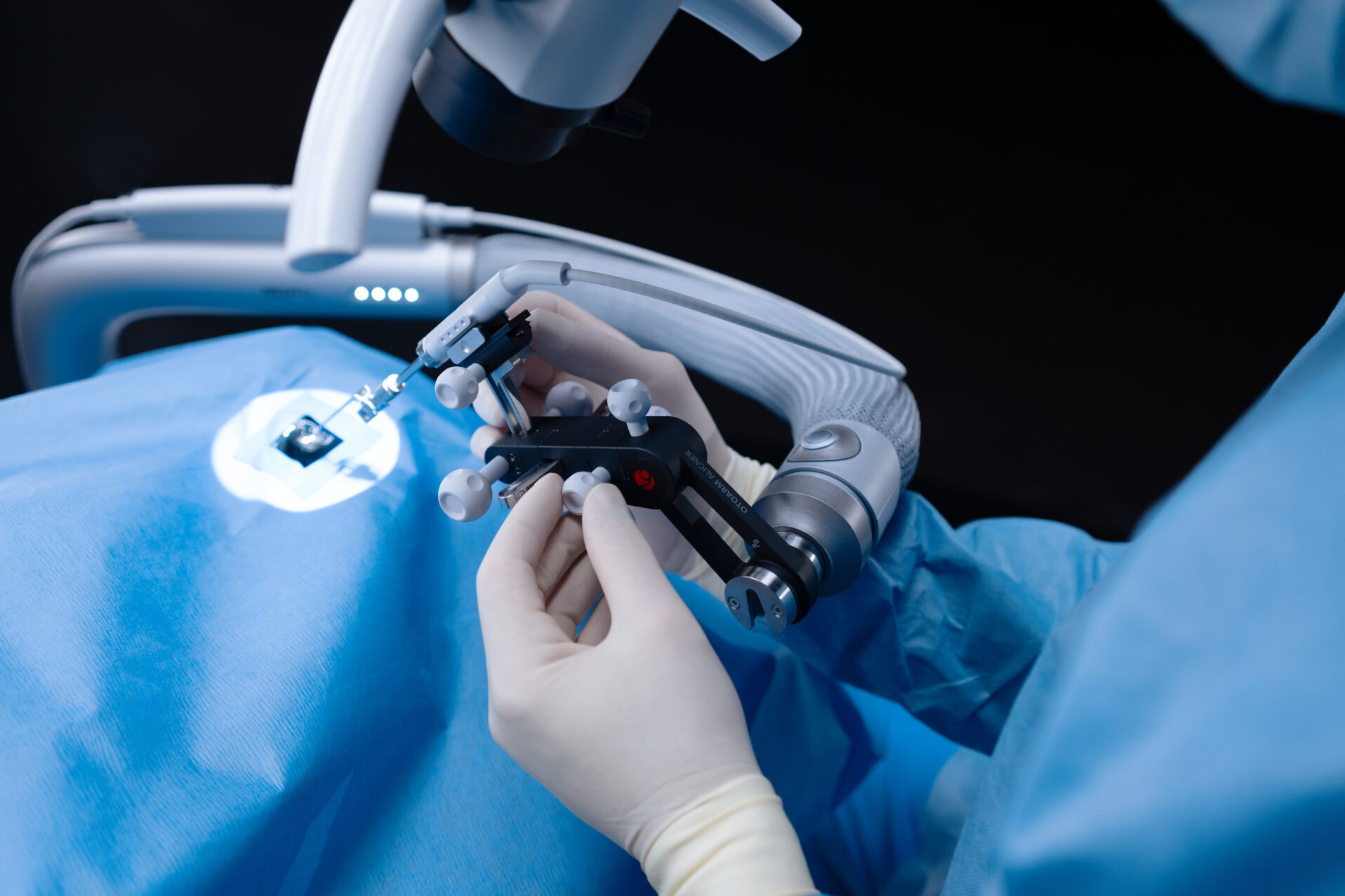
Photo: Otoarm Otodrive ©MED-EL
The results so far are promising: about 90% of the treated children show age-appropriate language acquisition, with very few side effects.[4] However, therapy is still in the phase of clinical studies, with very small numbers of cases. It is not yet clear when the therapy will be generally approved and available. Gene therapies for other genetic hearing disorders are even less advanced.
Future-ready with CI – also for future forms of therapy
To potentially benefit from therapies that may become available in the future, people affected today should:
- acquire and maintain the ability to speak
- preserve structures in the inner ear
With current cochlear implants and modern surgical technology, both are possible.
To preserve inner‑ear structures during cochlear implantation, the following are essential:
- Atraumatic electrodes – best FLEX electrodes[5]
- A large electrode selection, for the individually optimal electrode length[6]
Regardless of potential future gene therapy, children for whom a cochlear implant is indicated should be genetically tested:
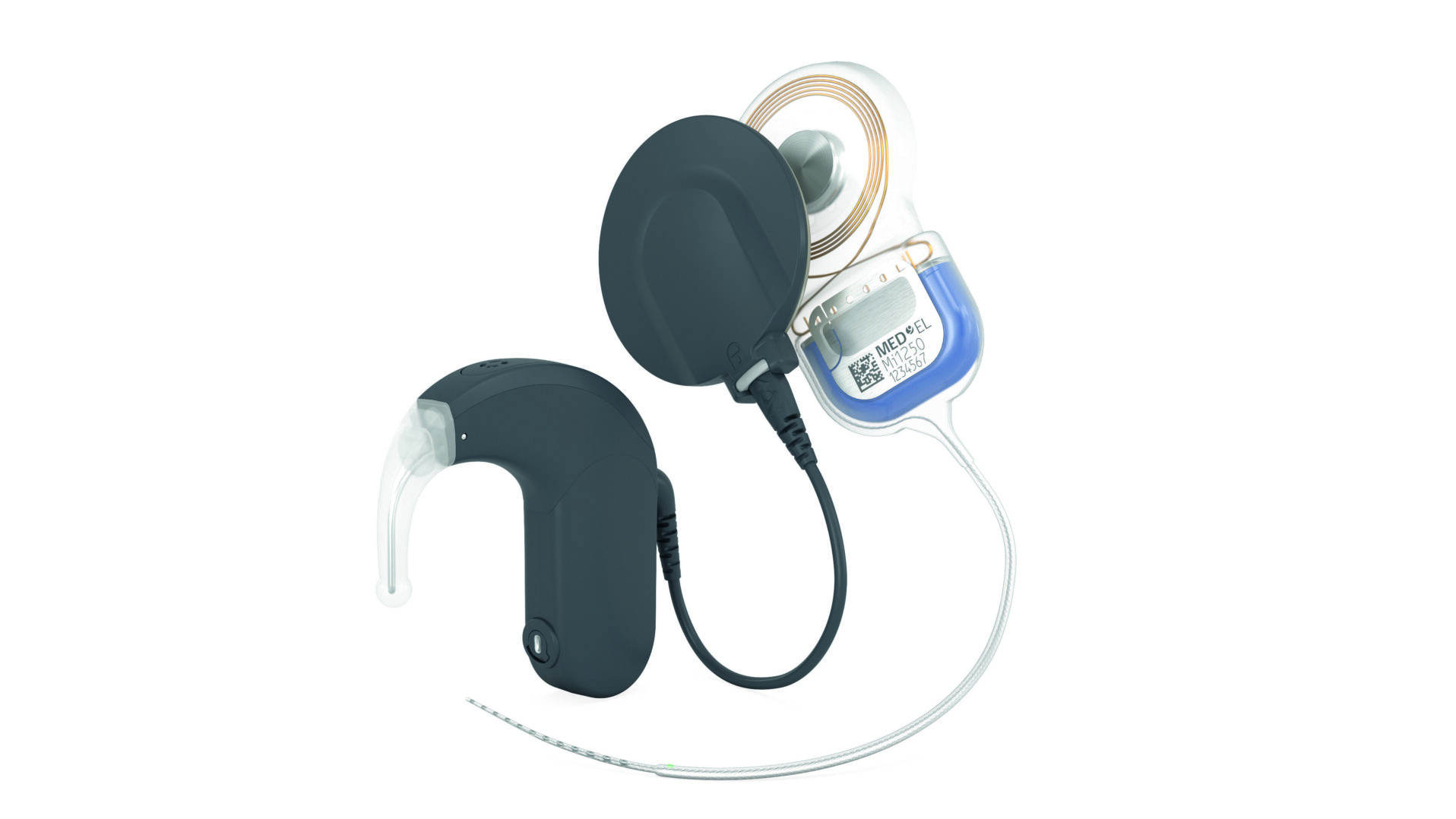
Photo: Synchrony 2_53 mini ©MED-EL
- to determine the cause of the hearing disorder
- to detect and take into account possible syndromes at an early stage
- to provide a prognosis for the progression of hearing loss and expected hearing outcomes
Therefore, genetic diagnostics should be an integral part of modern hearing rehabilitation without postponing cochlear implantation.
______________________________________________________________________________________________________________
[1] Birgit May-Mederake et al., Evaluation of auditory development in infants and toddlers who received cochlear implants under the age of 24 months with the LittleARS Auditory Questionnaire, International Journal of Pediatric Otorhinolaryngology 74 (2010) 1149–1155, doi:10.1016/j.ijporl.2010.07.003; Ona B.Wie, Language development in children after receiving bilateral cochlear implants between 5 and 18 months, International Journal of Pediatric Otorhinolaryngology, Volume 74, Issue 11, November 2010, Pages 1258-1266, doi.org/10.1016/j.ijporl.2010.07.026; and many more
[2] Litovsky R., Chapter 3 - Development of the auditory system, Editors: Aminoff M.J., Boller B., Swaab D.F., Handbook of Clinical Neurology, Elsevier, Volume 129, 2015, p.55ff, ISSN 0072-9752, ISBN 9780444626301, https://doi.org/10.1016/B978-0-444-62630-1.00003-2.
[3] Lin, F. R., & Albert, M. (2014). Hearing loss and dementia – who is listening? Aging & Mental Health, 18(6), 671–673. doi.org/10.1080/13607863.2014.915924; Polonenko M.J., Papsin B.C., Gordon K.A., Delayed access to bilateral input ages cortical organization in children with asymmetric hearing, NeuroImage: Clinical, Volume 17, 2018, p. 415-425, ISSN 2213-1582, doi.org/10.1016/j.nicl.2017.10.036; Polonenko, M.J., et al. Cortical organization restored by cochlear implantation in young children with single sided deafness. Sci Rep 7, 16900 (2017). doi.org/10.1038/s41598-017-17129-z; Sharma, A., et al. (2016). Cortical Plasticity and Reorganization in Pediatric Single-sided Deafness Pre- and Postcochlear Implantation: A Case Study. Otology & neurotology: official publication of the American Otological Society, American Neurotology Society [and] European Academy of Otology and Neurotology, 37(2), e26–e34. doi.10.1097/MAO0000000000000904
[4] Hearbetter - Interview with Arnoldner – coming soon
[5] https://blog.medel.pro/en-us/cochlear-implants/fda-expands-med-el-criteria-for-adults-with-residual-hearing/,
[6] https://blog.medel.com/technology/cochlear-implant-individualization-with-otoplan/






